Every year in France, 45,000 people have a thyroidectomy (total or partial removal of the thyroid gland). A common but delicate operation due to the proximity of the recurrent laryngeal nerves to the parathyroid glands.
A randomized clinical trial conducted between September 2016 and October 2018 in a series of 241 patients demonstrated the efficacy of autofluorescence imaging to preserve the parathyroid glands during surgery and thereby to reduce the rate of early postoperative hypocalcemia. Here are some key insights from that study.
In fact, parathyroid gland identification in the operating room can be a real challenge for the surgeon, who must operate with extreme precision in order to avoid inadvertently damaging the parathyroid glands. Accidental injury can cause postoperative hypocalcemia (a common complication which usually appears 24 to 48 hours after surgery). Today, thanks to advances in medical imaging, especially systems that use near infrared autofluorescence to identify the parathyroid glands in real time, the risk of hypocalcemia is considerably reduced.
Hypocalcemia after thyroidectomy: a frequent complication
In the operating room, the identification and preservation of the parathyroid glands during a thyroidectomy is a complex exercise, even for the most skilled surgeons. Because of their small size (2 or 3 millimeters in diameter), these glands may be accidentally damaged or excised, resulting in postoperative hypocalcemia (abnormally low level of calcium in the blood).
This type of complication affects nearly 30% of patients. It requires medical treatment with calcium supplementation for a period of 1 month to 1 year.
In very rare cases (1 to 4% of patients), hypocalcemia can be permanent, which severely impacts the patient’s quality of life.
Identification of the parathyroid glands and preservation of their vascularization during surgery is the only way to lower the risk of hypoparathyroidism. Nevertheless, despite all the efforts made in this area, the risk of unintentional trauma remains common.
A successful clinical trial for FLUOPTICS©
Between September 2016 and October 2018, a randomized clinical trial was conducted in 3 French hospitals in a total of 241 patients who underwent total thyroidectomy (with or without lymph node dissection). Patients were divided into two separate groups (120 + 121).
This allowed a comparison between an experimental group for which thyroidectomy was performed with the use of autofluorescence imaging and a “control” group which had a conventional thyroidectomy (without autoflourescence).
All interventions were performed by experienced surgeons.
In the “control” group, the parathyroid glands could be preserved when they were visible.
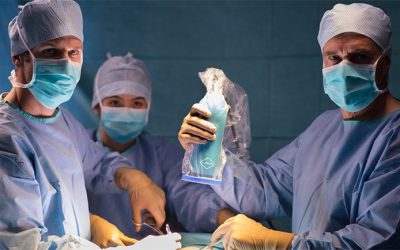
In the experimental group, the surgeon used the FLUOBEAM® 800 imaging system from FLUOPTICS© to examine the lobes of the thyroid. This technology allowed the surgeon to detect the parathyroid glands by autofluorescence in real time.
In this study, the use of autofluorescence led to a reduction in the rate of temporary postoperative hypocalcemia from 22% to 9%, by making it possible to better identify the parathyroid glands and thus better preserve them.
The main benefits of autofluorescence for patients and surgeons:
- Improved quality of the intervention;
- Precision of the surgical workflow;
- Preservation of parathyroid gland function.
To evaluate the effectiveness of the peroperative autofluorescence imaging system (NIRAF: near-infrared autofluorescence) during a total thyroidectomy (with lymph node dissection), patients were divided into two groups of 120 and 121 patients.
Analysis of the results shows that the rate of temporary postoperative hypoglycemia was 9.1% in the experimental group (11 of 121 patients) and 21.7% in the “control” group (26 of 120 patients).
The rate of parathyroid autotransplantation was 3% and 13%, respectively, and the rate of unintentional parathyroid excision was 2.5% versus 12%.
The rate of permanent hypocalcemia was 0% in the experimental group compared to 1.6% of patients in the “control” group (2 of 120 patients
Fluorescence imaging (NIRAF): an innovation that minimizes complications after thyroidectomy
The FLUOBEAM® 800 medical imaging system provides relevant images in real time. Parathyroid tissues emit an autofluorescent signal during surgery, allowing accurate visualization so as to preserve their vascularization during thyroid dissection. Thus, the risk of surgical trauma is reduced because the parathyroid glands are preserved. The result: the rate of temporary postoperative hypocalcemia is considerably reduced.
Autofluorescence helps to reduce the rate of postoperative hypocalcemia
Patients were followed by their doctor for 6 months in order to accurately assess the rate of permanent hypoparathyroidism.
Based on the clinical results, the experimental group (FLUOBEAM® 800) had a significantly lower rate of postoperative hypocalcemia (9%) than the control group (22%).
Two patients in the “control” group had permanent hypocalcemia, compared to none in the experimental group.
In addition, the rate of parathyroid autotransplantation was 3.3% in the experimental group compared to 13.3% in the “control” group.
FLUOBEAM® 800 imaging system: a breakthrough innovation for endocrine surgery
This clinical trial demonstrated the efficacy of the FLUOBEAM® 800 imaging system in endocrine surgery. It prevents the occurrence of hypocalcemia following total thyroidectomy (for thyroid cancer, multinodular goiter, Graves disease).
Throughout the surgery, this device makes it possible to better identify the parathyroid glands while preserving their functions. These small glands measuring just a few millimeters can be very difficult to detect with the naked eye. Surgeons must work harder to stay focused and avoid accidentally damaging them. Thanks to the FLUOBEAM® 800 system, the surgeon can better focus his/her attention in order to mentally plan the best thyroid resection for the patient.
Since this study was conducted, FLUOPTICS has gone further with the development of FLUOBEAM® LX entirely dedicated to thyroid surgery for enhanced ergonomics and to further improve the quality of parathyroid gland visualization in real time. Learn more about FLUOBEAM® LX.
This study demonstrates the clinical efficacy of autofluorescence in thyroid surgery, a true breakthrough for endocrine surgery. The results show that the use of the FLUOBEAM® 800 imaging system significantly reduces the risk of temporary postoperative hypocalcemia after total thyroidectomy. A reliable protocol that accompanies the surgeon throughout the surgery, making surgery safer and improving the identification and preservation of the parathyroid glands.