LYMPHATIC SURGERY
Discover FLUOBEAM® LMMETHODOLOGICAL APPROACH AND OPERATING STRATEGY WITH FLUOBEAM® LM?
After an interstitial injection, indocyanine green (ICG) is drained to the nearest lymph node chain. In lymphatic surgery, ICG fluorescence allows to visualize the superficial drainage and to identify the areas where functional lymphatic vessels and blockages are located. This allows a good understanding A good evaluation of the disease’s progression and to eventually plan a surgery in which fluorescence will help identify the critical areas where to perform lymphatic-venous anastomoses.
Another application of fluorescence in lymphatic drainage is the identification of sentinel lymph nodes in cancer surgery.. In axillary lymph node biopsy, this technique should benefit patients who do not have access to isotope detection. This technique can also be used in reverse mapping when we want to remove nodes and preserve those that drain nearby areas.
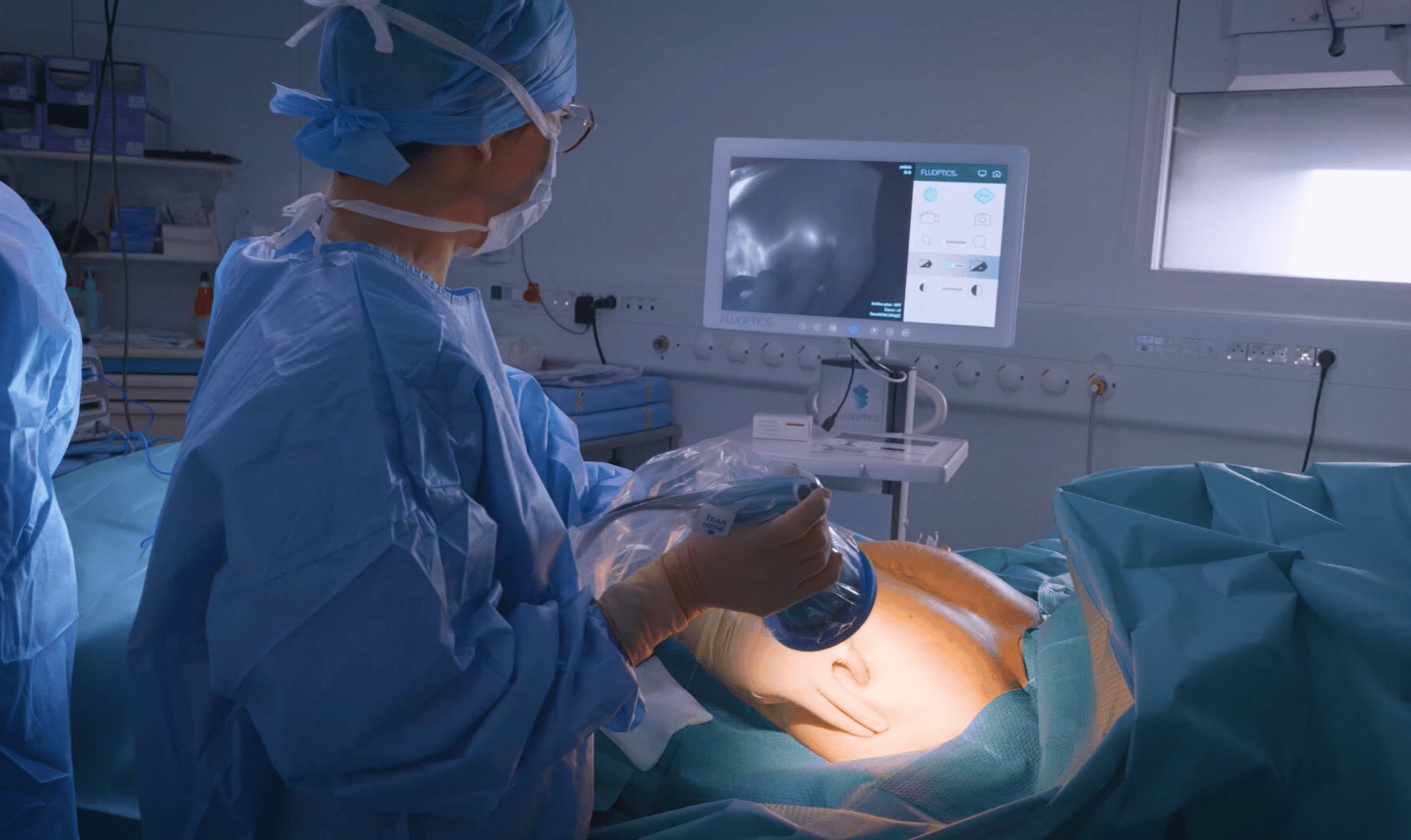
Fluobeam® LM in action
Observation of lymphatic vessels
In consultation, FLUOBEAM® LM can be used for real-time imaging of functional superficial lymphatic vessels. It helps in the early diagnosis of lymphedema, in the choice of treatment (surgical or medical), and in the postoperative follow-up.
In surgery, FLUOBEAM® LM can be used to identify before and during surgery the functional lymphatic vessels that will be used for a lymphatic-venous anastomosis (LVA). In addition, FLUOBEAM can be used in “reverse mapping” to map and preserve lymphatic drainage during lymph node surgery and can also be used for postoperative follow-up.
Observation of lymphatic vessels
In consultation, FLUOBEAM® LM can be used for real-time imaging of functional superficial lymphatic vessels. It helps in the early diagnosis of lymphedema, in the choice of treatment (surgical or medical), and in the postoperative follow-up.
In surgery, FLUOBEAM® LM can be used to identify before and during surgery the functional lymphatic vessels that will be used for a lymphatic-venous anastomosis (LVA). In addition, FLUOBEAM can be used in “reverse mapping” to map and preserve lymphatic drainage during lymph node surgery and can also be used for postoperative follow-up.
Sentinel node biopsy
The sentinel lymph node is the first lymph node where cancer cells are most likely to migrate from the primary tumor. The sentinel node technique involves detecting this node, removing it and having it analyzed.
Fluorescence imaging and Indocyanine Green have been recently introduced in the clinic as an alternative for surgical guidance. FLUOBEAM® LM allows visualization of superficial lymphatic drainage and detection of the sentinel lymph node after incision, for different tumor types.
Sentinel node biopsy
The sentinel lymph node is the first lymph node where cancer cells are most likely to migrate from the primary tumor. The sentinel node technique involves detecting this node, removing it and having it analyzed.
Fluorescence imaging and Indocyanine Green have been recently introduced in the clinic as an alternative for surgical guidance. FLUOBEAM® LM allows visualization of superficial lymphatic drainage and detection of the sentinel lymph node after incision, for different tumor types.
TESTIMONIALS
"Indocyanine green can be used in sentinel node detection in early breast cancers. It is an accurate, safe and inexpensive technique."

Dr Charlotte NGO
"It is essential to understand lymphedema works so FLUOBEAM® is really important for this kind of indication. I can't do lymphatic surgery without fluorescence imaging."

Pr Jaune MASIA
DISCOVER THE WEB MASTERCLASS
Don’t miss the opportunity to interact live with an expert in fluorescence imaging and ICG angiography applied to sentinel lymph node surgery. Register for a free one-hour session to discover or refine your knowledge.
PUBLICATIONS
FLUOBEAM® LM is indicated to visualize on a screen the flow, the distribution and/or the accumulation of Indocyanine green (ICG) before, during and after surgery for the indications such as: visualization of the blood flow, visualization of the lymphatic flow, visualization and identification of the bile ducts during hepatobiliary surgery, visualization and detection of primary liver tumors and/or hepatic metastases.FLUOBEAM® LM is also indicated to facilitate the visualization of parathyroid glands by auto-fluorescence (natural fluorescence without ICG injection) during thyroid and parathyroid surgeries. This is a class IIa medical device, CE017. Product manufactured by FLUOPTICS SAS, France. For proper use, please read carefully all instructions in the specific instructions for use for each product.