Fatigue, weight loss, hot flushes, palpitations, brittle nails, etc. all these signs may mean that you have a thyroid disorder (hyperthyroidism or hypothyroidism). In France, thyroid disorders affect 10% of the population. This tiny gland located at the base of the neck secretes hormones that regulate many vital functions including heart rate, digestion, etc. Some symptoms can serve as a warning to see a doctor. The earlier a thyroid disorder is diagnosed (via a blood test), the sooner it can be treated. Here are the signs of a thyroid condition.
What are the symptoms of hyperthyroidism?
Hyperthyroidism is a disorder related to a dysfunction of the thyroid gland, a butterfly-shaped endocrine gland located at the base of the neck. Hyperthyroidism has different causes, the most common (75-80% of cases) being Graves’ disease, an auto-immune disorder, which mainly affects women and results in an over-production of thyroid hormones.
Symptoms that may indicate potential hyperthyroidism:
- Persistent fatigue;
- Unexplained weight loss;
- Excessive thirst;
- Oversensitivity (irritability);
- Insomnia;
- Diarrhea;
- Heart palpitations and tremor;
- Bulging eyes;
- Visible goiter, due to enlargement of the thyroid gland;
- Irregular heartbeat;
- Hot flushes;
- Polycystic ovary syndrome (hypothyroidism/hyperthyroidism).
All these symptoms may indicate that your thyroid is overactive. Hyperthyroidism can be caused by a number of factors including a benign tumor in the thyroid gland, thyroid cancer, a toxic nodule or a goiter.
What are the symptoms of hypothyroidism?
Hypothyroidism is a thyroid disorder related to a deficiency of thyroid hormones. The secretion of thyroid hormones (T3 and T4) is regulated by the pituitary gland, which produces TSH (Thyroid Stimulating Hormone). The result: metabolism is slowed down.
After the age of 50, women are more exposed to the risk of hypothyroidism.
Here are the main symptoms of hypothyroidism:
- Persistent fatigue;
- Unexplained chilliness (always feeling cold);
- Unexplained weight gain;
- Decreased appetite;
- Slowed heart rate;
- Elevated blood cholesterol level;
- Painful joints, muscle aches;
- Changes in menstrual patterns;
- Unusual constipation;
- Presence of a goiter (enlarged thyroid gland);
- Puffy face, bulging eyes;
- Irritability;
- Difficulty concentrating, impaired memory;
- Dry skin (possibly with redness);
- Fragile, brittle nails;
- Hair loss;
- Hoarse or cracked voice.
When the thyroid doesn’t produce enough hormones, there can be a number of causes:
- Hashimoto’s disease (which leads to destruction of the gland). Hashimoto’s thyroiditis is the most common cause;
- Iodine deficiency;
- Post-operative complication of a thyroidectomy (removal of the thyroid gland);
- Some medications.
Congenital hypothyroidism is a disorder related to abnormal functioning of the thyroid gland right from birth. In developed countries this disorder affects 1 in 3,000 newborns.
Some cases of mild hypothyroidism can be treated with natural precursors of thyroid hormones which are very effective and avoid the side effects of certain thyroid medications.
Palpation of the neck to better detect the signs
Palpation of the base of the neck is the first step in a thyroid exam to detect any thyroid abnormalities, before referral for an ultrasound.
Palpation of the thyroid gland is done while the patient is seated. The physician gently places his or her hands on both sides of the neck, under the jaw, then slides the fingers downward to the base of the neck where the thyroid gland is located.
The purpose of palpation is to assess the symmetry of the gland and detect any possible enlargement.
The physician then palpates the anterior and posterior cervical lymph nodes.
Thyroid: when is it necessary to operate?
Thyroidectomy involves making a small incision at the base of the neck. The need for surgery (thyroidectomy) can arise in two situations: when medication alone does not succeed in stopping enlargement of the gland (causing problems with swallowing), and when there is a toxic nodule (symptoms of thyroid cancer).
Surgery for suspicious nodules involves removing all or part of the thyroid gland.
Before surgery, the physician orders several exams including an ultrasound and Doppler (to assess the vascularization of toxic nodules and for cytological puncture).
When is surgery needed?
- A large nodule measuring more than 4 cm;
- Presence of several nodules forming a goiter;
- Nodule filled with fluid;
- When a risk of thyroid cancer is suspected.
In some thyroid cancers, radioactive iodine therapy is recommended to complete the surgery.
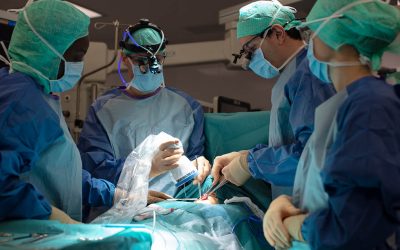
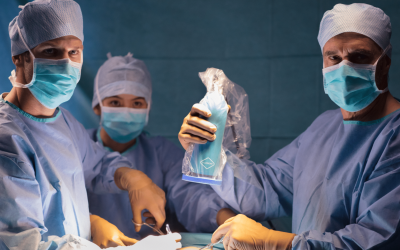
What are the benefits of the new FLUOBEAM® LX?
In the field of endocrine surgery, significant progress has been made in medical imaging. The new FLUOBEAM® LX is an innovative system designed to improve the quality of thyroid surgery. Developed by FLUOPTICS©, the FLUOBEAM® LX is a state-of-the-art imaging system enabling surgeons to clearly see the parathyroid glands in real time thanks to the autofluorescence of these glands.
This innovative protocol allows surgeons to first identify the parathyroid glands so as to locate them and preserve them during resection of the thyroid.
The surgeon may also decide to inject indocyanine green during surgery to locate the vessels that perfuse the parathyroid glands, and thereby preserve their vascularization during thyroid resection.
Lastly, at the end of surgery the surgeon can check the perfusion of the parathyroid glands using another injection of indocyanine green.
With a sensitivity, specifically adapted to detect low level of fluorescence intensities, the FLUOBEAM® LX provides surgeons with clear, precise information to better meet medical needs and operate in the best possible conditions.
Each year, 45,000 people undergo thyroid surgery, a common procedure but one which has certain risks, such as hypocalcemia. Thanks to the progress made by FLUOPTICS© in the field of medical imaging, the rate of postoperative complications of thyroidectomy has dropped from 20 to 5%. With this innovative system, surgeons have a reliable, easy to use tool enabling them to clearly and accurately identify the parathyroid glands and avoid inadvertently damaging or excising them.