Hypoparathyroidism is characterised by insufficient production of the parathyroid hormone (PTH), a hormone secreted by the parathyroid glands which plays an essential role in the regulation of serum calcium level. Low levels of PTH can cause hypocalcaemia (abnormal decrease of blood calcium levels) and increased phosphorus levels in the body.
Patients will present fairly incapacitating symptoms such as muscle spasms, depression and lethargy. To help patients recover their quality of life, treatment is essential to stabilise blood calcium levels. Diagnosis and treatment… Here are a few tips to prevent hypoparathyroidism.
Hypoparathyroidism: definition and treatments
What is hypoparathyroidism?
There are three main causes of hypoparathyroidism:
- Post-surgical: following thyroid surgery or parathyroidectomy;
- Genetic;
- Idiopathic: a PTH secretion deficiency may occur at any time, especially with conditions such as chronic kidney failure, vitamin D deficiency, etc.
The most common cause by far (in 75% of cases) is post-surgical hypoparathyroidism (damage to the parathyroid glands after undergoing thyroidectomy to treat thyroid cancer or a goitre, or after parathyroidectomy or radioactive iodine treatment).
However, in rare cases it can have a congenital (DiGeorge syndrome, velocardiofacial syndrome which affects 1 in 4000 births) or idiopathic cause and may develop at any stage of life.
Hypocalcaemia, caused by hypoparathyroidism, results in an abnormal decrease in blood calcium levels due to excessively low secretion of PTH (parathyroid hormones), which is responsible for bone resorption.
Consequence: kidneys can longer function due to the PTH deficiency; it reabsorbs large amounts of phosphate (hyperphosphoremia) and also stops reabsorbing calcium.
Main clinical signs associated with hypoparathyroidism:
The effects of hypoparathyroidism are particularly severe and incapacitating for patients:
- Neuromuscular manifestations: tetanus (70% of cases), contractures, cramps, perioral paraesthesia (affecting the lips), distal paraesthesia (hands and feet);
- Cardiac disorders: arrhythmia, conduction disorders;
- Psychological disorders: mood swings, irritability, psychosis, anxiety, depression;
- Eye manifestations: cataracts affect 13% of people with hypoparathyroidism;
- Dermatological manifestations: dry skin, dry and fine hair, weak and brittle nails, degradation of dental enamel, candidiasis.
Hypoparathyroidism: current treatments
Hypoparathyroidism is a condition that is often difficult to diagnose. Diagnosis is only confirmed by measuring PTH, calcium and phosphorus levels.
To treat post-surgical hypoparathyroidism, calcium and vitamin D supplements are essential to restore normal serum calcium levels. Vitamin D helps promote the absorption of calcium.
Patient care may vary between establishments and the range of treatments includes:
- Low doses of calcium;
- Active form of vitamin D (calcitriol or Alfacalcidol) to promote calcium absorption in the kidneys and intestines.
In cases of severe hypocalcaemia, calcium is administered parenterally (by injection), intravenously or by infusion.
Patients require regular check-ups (several times a week at the start of treatment) to control blood calcium levels. After serum calcium levels have stabilised, a visit every 3 to 6 months is usually sufficient.
Good to know:
Vitamin D deficiency leads to calcium and phosphate metabolism disorders (in case of chronic kidney failure) which can increase cardiovascular risks and trigger Fahr syndrome – a condition characterised by the calcification of the central nuclei. It is therefore important to monitor vitamin D levels.
Can post-thyroidectomy complications be avoided?
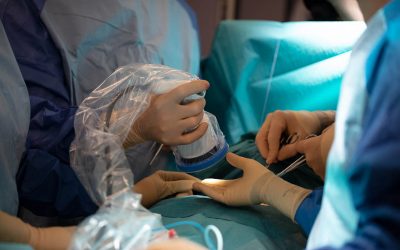
During thyroid surgery, identifying the parathyroid glands can be a real challenge, even for an expert surgeon, due to their small size. These glands may be damaged involuntarily due to the problems in identifying them during surgery, which may result in postoperative hypoparathyroidism.
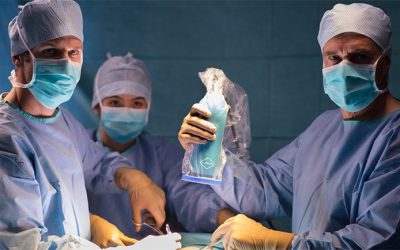
Thanks to fluorescence imaging, it is now possible to significantly improve the visibility of the practitioner and thus reduce the risk of hypocalcaemia after surgery.
FLUOPTICS©, a French company specialising in the development of fluorescence imaging devices, has developed FLUOBEAM® LX, a fluorescence imaging system exclusively designed for parathyroid imaging. This device allows the visualisation of the parathyroid glands in autofluorescence (natural fluorescence).
Thanks to the autofluorescence of the parathyroid glands, surgeons can better locate these glands in real time and, with FLUOBEAM® LX, they benefit from optimal comfort of use (fluid images, adapted depth of field) as well as a unique level of sensitivity.
In Europe and the USA, the number of practitioners who have adopted it is rising steadily (over 500 surgical procedures have been performed up to now using this system).
Hypoparathyroidism is a condition that can cause serious complications. It manifests as hypocalcaemia and hyperphosphoremia – conditions that require lengthy and even sometimes lifelong medical care. PTH replacement treatments reduce symptoms but require the strict monitoring of patients. Thanks to FLUOBEAM® LX, a new medical imaging device entirely dedicated to thyroid surgery, practitioners can accurately visualise the parathyroid glands in real time and improve the precision of their actions, thus avoiding unintentional damage to these glands which can result in postoperative hypocalcaemia and affect the quality of life of patients.